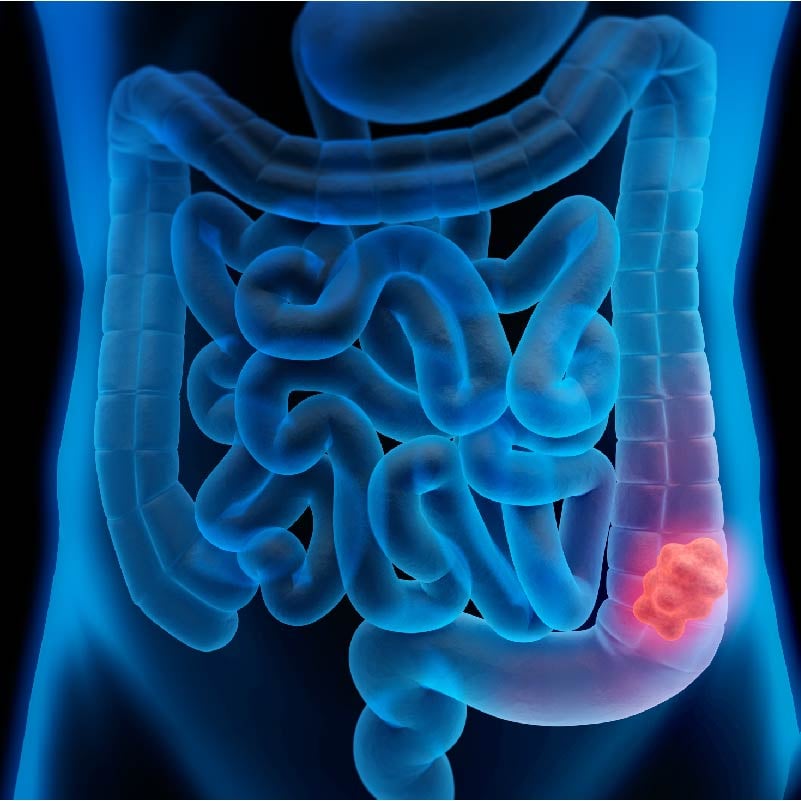
Colorectal cancer is the third-most common type of cancer diagnosed each year in the United States, excluding skin cancers.
Thankfully, increased rates of screenings have helped to lower the overall number of people diagnosed with colorectal cancer over the last 20-30 years.
Asim Mushtaq, MD, is a gastroenterologist with Rochester Regional Health and describes the various screenings available and why patients may want to choose one over another.
What is the purpose of a screening?
First, it may help to know what providers are looking at during a screening. The colon and rectum are part of the gastrointestinal (GI) system. These two parts of the GI system make up the large intestine, which helps your body digest food.
The colon, which is about 5 feet long, processes salt and water from material that has already moved through your small intestine. Any waste is then transferred into the rectum, where it stays until it is ready to be excreted from your body via a bowel movement.
Screenings are conducted to detect pre-cancerous polyps (small growths on the inner lining of the colon or rectum) and early stage colorectal cancer before they become symptomatic.
Physicians will provide screenings for average risk patients, meaning the patients do not have a history of cancer or increased risks for cancer.
Currently, the recommended age to begin regular colorectal screenings is 45, according to the American College of Gastroenterology and U.S. Preventive Services Task Force. Previous recommendations had screenings start at age 50, but the age was lowered because of an increase in the number of colorectal cancer patients younger than 50.
In most cases, regular screenings will end by age 75. However, if a patient has a life expectancy beyond 10 years, they can have a conversation with their primary care provider about whether to continue with these screenings.
Types of colorectal cancer screenings
There are several methods of screening for colorectal cancer. Each one has its advantages and challenges. A conversation with your doctor is the best way to determine which is right for you.
A patient may choose a particular type of screening based on:
- Medical history
- Sensitivity
- Specificity
- Frequency of testing
- Location at which screening is offered
There are two main branches of testing: stool-based tests and endoscopic tests.
Stool-based tests are much more sensitive for detecting cancer and less sensitive for detecting pre-cancerous polyps. There is the possibility of a false positive with some of these tests, which providers take into account.
gFOBT (guaiac fecal occult blood test)
How it works: A patient will obtain samples from 3 consecutive bowel movements at home and bring it to their primary care provider. Using a specialized stool card, the samples are then tested to detect if there is evidence of microscopic bleeding.
Frequency: Once a year
FIT (fecal immunochemical test)
How it works: This is the most-frequently chosen option for stool-based tests. A patient will bring a small sample to their primary care provider. The sample is then sent to a lab, where it is tested for hemoglobin. Hemoglobin is an early indicator of new tissue growth in the colorectal area of the body.
Frequency: Once a year
DNA stool test (Cologuard®)
How it works: A patient will obtain a sample from a full bowel movement and ship it to a lab. Providers will test the sample for certain molecules and look for DNA mutations that indicate potential growths.
Frequency: Once every 3 years.
Endoscopic tests use a thin, flexible tube fitted with a tiny light and camera to see inside your body. These tests are highly sensitive for detecting colorectal cancer and non-cancerous polyps. Patients are sedated in nearly all cases to minimize any discomfort.
An endoscopic test allows for detection of any polyps, and removal of pre-cancerous polyps all during a single test.
There are tradeoffs to these types of tests. They are more invasive than stool-based testing and they require some preparation by the patient to empty the colon and rectum ahead of time.
Colonoscopy
How it works: For most patients, this is the first option for an endoscopic screening. A provider will examine the patient’s rectum and colon using a colonoscope, which is inserted through the anus and fed upward through the colon.
Frequency: Once every 10 years – depending on findings from the exam
Sigmoidoscopy
How it works: Entering through the anus, a provider uses a sigmoidoscope to examine the rectum and part of the lower colon called the sigmoid colon. If a sigmoidoscopy shows polyps, a colonoscopy may be recommended as the next step to examine the remainder of the colon.
Frequency: Every 5 years – depending on findings from the exam
Colon capsule endoscopy
How it works: A patient swallows a capsule containing two tiny cameras. The capsule travels through the gastrointestinal system, passing through the colon and rectum. The cameras are then taken by providers and any recordings are analyzed for potential issues.
Frequency: Only for use by patients who had incomplete colonoscopies
CT Colonography (virtual colonoscopy)
How it works: This procedure is performed by a radiologist. After preparation to empty the colon and rectum, a patient will undergo a CT scan and have X-rays taken of their colon and rectum. The patient does not need to be sedated with this method of screening.
Frequency: Only for use by patients who cannot have complete colonoscopies for medical reasons
Another method of screening that does not fall under the stool-based or endoscopic categories is the double-contrast barium enema.
Double-contrast barium enema
How it works: After 24 hours of preparation by the patient to clean the colon, an X-ray is used in conjunction with a liquid barium solution to produce clear x-ray images of the lower GI tract. If something abnormal is detected, an additional test may be required for further examination.
Frequency: Every 5 years – depending on the findings of the exam
Next steps
If one of these stool-based tests comes back positive, the next step would be to get a colonoscopy.
Once a provider completes the colonoscopy, they will assess the results and work with the patient to determine what comes next.
“Depending on what the provider sees during the exam, they will recommend more surveillance, an additional colonoscopy, or a specific course of treatment,” Dr. Mushtaq said.
Staying in the know
Knowing what to do and when to do it is half of the battle with colorectal cancer screenings. For most patients undergoing screenings, Dr. Mushtaq said they stemmed from a conversation with their primary care provider.
Patients who may be referred to a gastroenterologist often are experiencing other gastrointestinal symptoms. If they are referred by their primary care provider, there is a better chance of catching something early that could have ended up being harmful if left alone for too long.
Having a good provider-patient relationship is key to staying healthy.
“It is important for patients to be told by their primary care provider that they need to have a colorectal cancer screening starting at age 45,” Dr. Mushtaq said. “Primary care provider education is one of the most important ways of staying informed.”