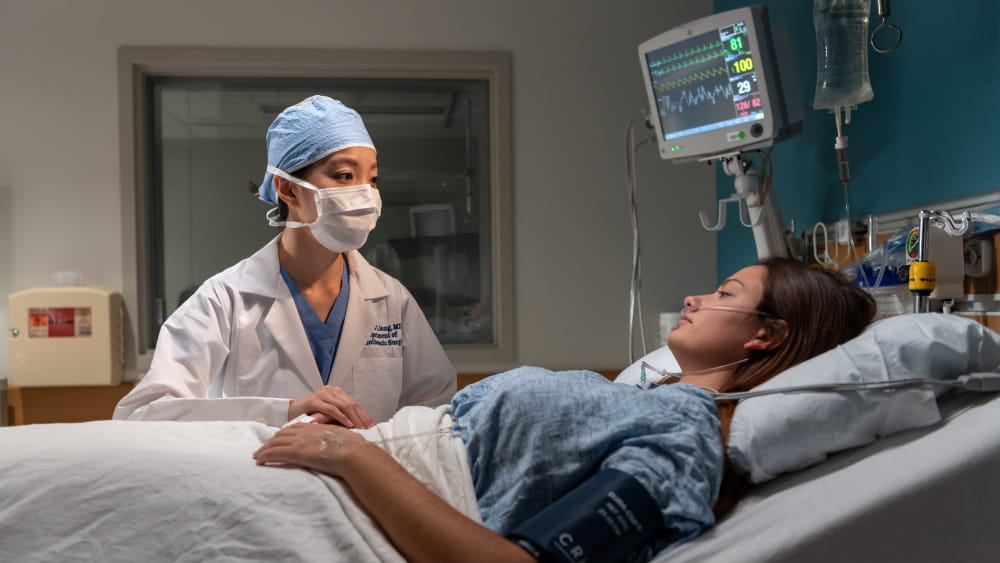
A diagnosis of lung cancer or other conditions that require surgery can be intimidating or overwhelming. The cardiothoracic surgical unit at Rochester Regional Health has one of the most experienced teams in Western New York and the greater Rochester region.
More and more often, surgeons are using robotic surgical systems to perform more complex operations. These operations have many benefits, ranging from being less invasive to having a quicker recovery time.
Veronica Shuyin Liang, MD, and Neal Chuang, MD, are two thoracic surgeons who have performed these procedures and explain how it works.
There are several reasons why patients want to consider a robotic-assisted thoracic surgery instead of an open surgery.
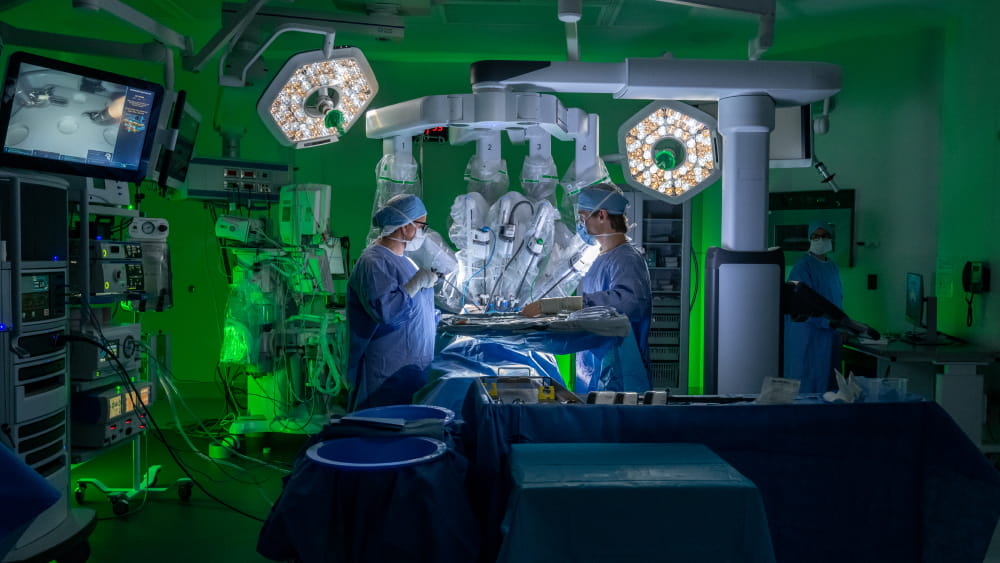
With a robotic surgery, the procedure is minimally invasive. The surgeon operating the robot makes a series of small incisions. An open surgery would involve opening up a patient at least 4-6 inches in order to see everything inside the chest cavity.
The robotic surgery’s small incisions and use of tiny cameras make the process minimally invasive and allows for a faster recovery. This also allows the surgical team to have more maneuverability during the operation and can allow more complex procedures to be completed.
“With the robot, you really get the magnification, the high-resolution view, three dimensional visualization, and then also the manual dexterity inside the chest to maneuver around the delicate blood vessels in the chest,” Dr. Liang said.
Most patients have a history of smoking and/or have been diagnosed with lung cancer. All ages and genders qualify for the procedure.
If lung cancer is the reason for the surgery, it has to be deemed “resectable” – or able to be operated on. This means it has to be a certain size and not near any main arteries and airways. This is the case with most early stage lung cancers, with no spread to remote sites of the body.
Rochester Regional Health was the first hospital system in the greater Rochester area to do a complete robotic esophagectomy – a procedure which removes either most of the esophagus and then reconstructs it using a portion of the stomach.
Drs. Liang and Chuang were the first surgeons in Rochester who have successfully performed sleeve lobectomies, complex re-do foregut procedures, and internal mammary artery harvest for coronary artery bypass graft (CABG) surgeries.
Rochester Regional Health began performing robotic thoracic surgeries at Rochester General Hospital and Unity Hospital in February 2020.
Since that time, more than 180 robotic thoracic surgeries have been performed between the two hospitals.
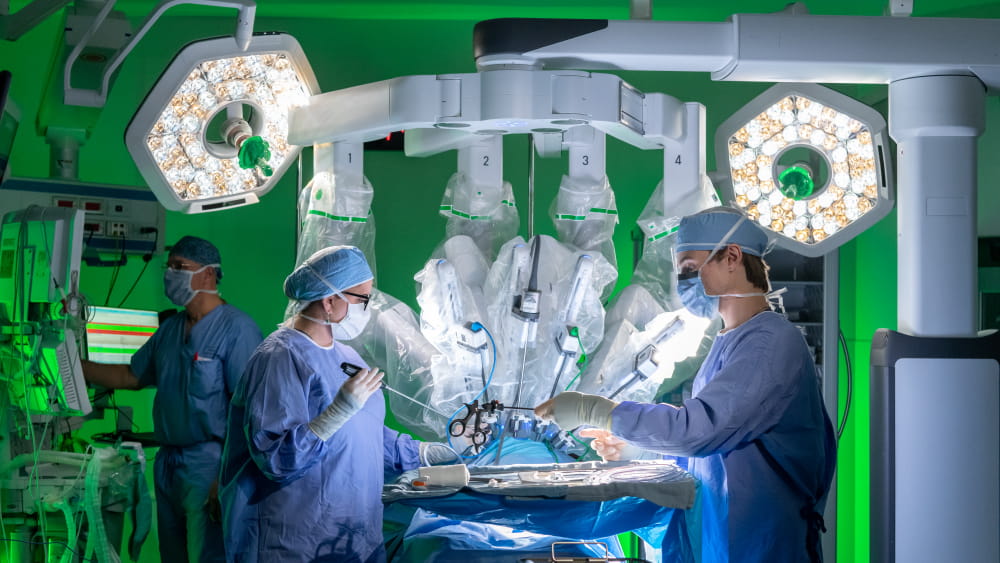
Robot-assisted thoracic surgeries are being done at two locations in Rochester: Rochester General Hospital and Unity Hospital.
As more people continue to learn about robot-assisted surgeries at Rochester Regional Health, the number of patients has continued to rise over the last 18 months. More than twice as many robot-assisted thoracic surgeries are taking place at Rochester Regional hospitals than any other hospital system in the region.
Surgeons are required to perform five procedures before they can operate without a mentor or supervisor present. A team of physician assistants, nurses, scrub technicians, and anesthesiologists are also trained to be part of the operation.
“There are a series of modules that a surgeon has to go through just learning about the robotics system, how to operate the controls,” Dr. Chuang said. “There are also some simulations and exercises they should do. So there is a program that Intuitive [a training program run by da Vinci] has that you need to sign off and get certified. And then you actually start to do procedures on patients and it’s much better if you have a mentor like Dr. Liang was for me.”
Conversion rates are a good indicator of how good surgeons are at these procedures. A conversion occurs when a robot-assisted surgery needs to be switched to an open surgery due to abnormal anatomy, intraoperative emergency, or unexpected findings during the operation that requires a larger incision. Dr. Liang has a conversion rate around one percent, meaning 99 percent of patients have successful robot-assisted procedures.
Following an open surgery, patients typically stay 4-5 days in the hospital to recover before being discharged.
With a robotic surgery, the hospital stay is generally 1-3 days. After the surgery, a chest tube is put in place to drain fluid from the lungs as they heal. Once the tube is removed, the patient can go home.
For most non-smokers who have good functional status before the operation, they can go home as early as the next day.
“As the team gains more experience in minimally invasive surgery, patients develop less postoperative pain and faster recovery. For those who do not need additional therapy, they return to their baseline activity level or resume work sooner. For those who need additional therapy for cancer, they can start the therapy sooner,” Dr. Liang said.
As with most surgeries of the chest, patients are advised to avoid heavy lifting for two months. There is usually a period of one month before a patient can be completely back to their physical state before the surgery, depending on how active they are. The more active a patient was before the surgery, the faster they are likely to recover.