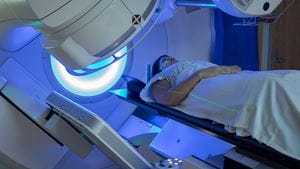
Among the various forms of treatment available for breast cancer patients is radiation therapy.
Treating some breast cancer patients with radiation is challenging because of how close some of the affected breast tissue can be to the heart muscle. Scientists have developed a number of therapies and treatments to help reduce the risk of heart issues – including different methods of radiation therapy.
Jeffrey Haynes, MD, is the Chair of Radiation Oncology at Lipson Cancer Institute with Rochester Regional Health and explains how a particular type of radiation therapy technology helps reduce the risk of heart issues.
Radiation therapy helps providers reduce the risk of cancer returning by killing any remaining cancer cells using high-energy rays in the area where cancer has been removed.
A patient will undergo a CT scan to determine exactly where the treatment needs to be focused, then will come in for treatment 2 weeks later. The CT scan creates a 3D model of the heart, lungs, breast, cavity where tumor was, and lymph nodes. The team then takes that knowledge and shapes the radiation beams to create a dose tailored to each patient.
On the day of a radiation session, patients lie down on a table under to the radiation machine so it can travel around the patient’s body, targeting the affected area with precision doses of radiation. One session lasts for about 15 minutes.
Patients do not feel anything during the treatment, but commonly experience redness and itchy skin afterward.
Radiation treatments are typically scheduled every weekday, lasting anywhere from 1-7 weeks – depending on the patient’s diagnosis. A radiation oncology physician will check in with the patient at least once a week to determine how the treatment is progressing.
Some patients being treated for cancer in their left breast undergo radiation therapy after surgery. During their radiation session, a small area in the corner of the heart can receive the same dose of radiation as the breast.
Applying the dose of radiation to this area of the heart slightly increases the risk of a patient having a heart attack, according to researchers.
Radiation oncologists at Lipson Cancer Institute are using an innovative technology from VisionRT called AlignRT® technology + the Deep Inspiration Breath Hold (DIBH) therapy. This method allows providers to track a patient’s breathing patterns with the goal of timing the radiation beams and eliminating damage to the heart.
“When a patient takes a deep breath in, it pulls the heart down and pushes the breast forward,” Dr. Haynes said. “The result is that it creates more space between the breast and the heart, allowing us to give the full cancer-killing dose to the breast with no effect on the heart.”
Rochester Regional Health is the only cancer center using this technology in Western New York, which has been proven to eliminate problems with oxygen flow in the heart (perfusion defects) that would otherwise be caused by radiation.
Since AlignRT®was first put in place at Lipson Cancer Institute in 2019, providers no longer see higher rates of heart attacks or heart failure.
When radiation oncology teams have a patient whose treatment puts them at an elevated risk for heart damage, they will get in touch with the cardiac oncology team at Sands-Constellation Heart Institute. Aligning these teams allows them to work closely with each patient with the shared goal of eliminating the risk of heart damage.
This collaborative planning approach extends to the radiation oncology team itself. Each morning, all of the radiation oncology physicians come together to review the patients’ cases and determine the best possible radiation target for every patient.
“By coming together every day, we can pool our collective knowledge to balance our goals of eliminating cancer and minimizing risks for the health of each of our patients,” Dr. Haynes said.
